For most Americans, mental fitness is a useful term, but mental fitness is not a scientific concept.
Many around the world questioned the results of a health exam last month and inclusion of a cognitive test for President Donald Trump. White House Physician Rear Admiral Dr. Ronny Jackson declared the president scored all answers correctly in his exam measuring mental fitness. For good reasons, mental health professionals have questioned the accuracy, comprehensiveness and motivation behind the physician’s public statement. Many also question claims by author Michael Wolff about the mental fitness of Trump in interviews concerning his blockbuster book, Fire and Fury: Inside the Trump White House.
This lay terminology of fitness is complicated and needs deconstruction. The vagueness of the terminology fosters confusion and needlessly strident debates. What’s more useful is to think of mental fitness as the “the fitnesses.” And there are many. It is best to consider the term in the context of people’s lives.
The concept of mental fitness might seem similar to physical fitness as both — for most of us — are aspirational. But there are important differences. Mental fitness is conflated with social, behavioral, developmental and occupational expectations. While for most people mental fitness means something in the cognitive realm — how well the brain is thinking, for instance — the term also implies emotional, temperamental and characterological dimensions.
The more salient question is: mental fitness for what?
Dr. Jackson reported that the president was in excellent cognitive health when he scored 30/30 on the Montreal Cognitive Assessment (MoCA). This is a commonly used cognitive screening test useful in medical settings to determine if further cognitive interrogation is warranted.
Confusion and altered awareness (known as delirium), memory deficits with reversible or irreversible brain deterioration (dementia), or localized brain lesions, are common findings that might trigger the need for more invasive neurologic testing such as CT, MRI, or PET scans.
The MoCA is a pencil and paper test that surveys brain functions such as language, attention, video-spatial orientation and short-term memory. A score above 26, in the absence of other symptoms, usually signals no further cognitive testing is warranted.
In people who were previously high functioning, this test may not detect meaningful decreases in cognitive functioning unbeknownst to the patient. These include early forgetfulness, name confusion, subtle disorientation, attention or perceptual deficits, to name a few.
The gold standard for cognitive testing is a neuro-psychology battery of tests performed by trained neuropsychologists. These tests can last several hours and are built on the rich intellectual foundation and detailed assessments of brain injuries by the Great Russian psychologist, Alexander Luria, during World War II.
He detected brain deficits by asking various questions and having the patient perform functions which mapped on to tissue-damaged brain areas. These exquisite tests predate neuroimaging of computerized axial tomography (CT) in the 1970s and magnetic resonance imaging (MRI) in the 1980s.
Sadly, the art of diagnosis based on detailed verbal interrogation of verbal and behavioral responses is being lost for today’s physicians. The study of the how the brain correlates to the mind goes back to Ancient Egypt.
The more well-known WAIS IV IQ test is often included in the battery. This is a so-called test of general mental agility or IQ which should be normalized for one’s population and age. Interesting the supposedly highly genetically influenced IQ has increased on average in the U.S. population over time.
This was dubbed by Charles Murray, of The Bell Curve fame, the Flynn Effect. James Flynn, Professor Emeritus at the University of Otago, scientifically refuted Charles Murray’s and Arthur Jensen’s (authors of Heritability of IQ, Race and Intelligence) belief that Black-white IQ gap are accounted by genetics. He has chronicled in great detail environmental influences that explain the gap.
As a psychiatrist with 30 plus years of experience working in medical/surgical hospital settings, I witness that one of the most questions posed is: does this patient have the mental fitness or “capacity” to make health care or legal decisions?
This question often involves the ability to consent to a medical procedure or determine his or her power of attorney for healthcare, that is can and cannot make health decisions when the patient can’t.This is a determination of mental fitness for the purpose of the ethical treatment of patients and respect for their autonomy. If they have capacity, they are generally free to make healthcare decisions that caretakers might feel are foolish or just plain wrong. Depending on the situation, it is not rare that a specialized judge might be called in to make a judicial decision of capacity, which is binding.
Mental fitness can be developmental and fluid over time. The same person may score differently on certain test at different eras of his or her life and due to different circumstances. For instance, in alcoholic treatment programs specializing in the treatment of professionals, often the question is: can this airline pilot return to flying planes, can this physician safely return to caring care for patients?
This is a mental fitness assigned for specific occupations. Because of the public health relevance of a return-to-duty clearance, these examinations are very thorough and the concept of mental fitness is elevated to a much higher threshold.
So a relevant question for all Americans now needs to be what should be the threshold for a sitting U.S. president — especially if real cognitive or emotional deficits are independently suspected. Although controversial, there were suspicions by some that President Ronald Reagan showed signs of senility before he left the office.
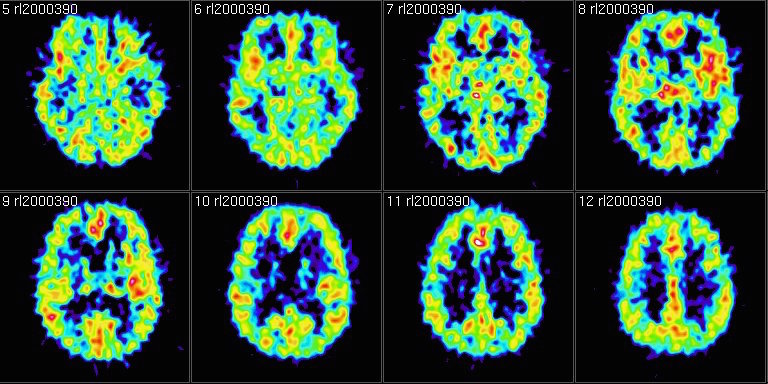
There is a palpable fear of cognitive decline in this epidemic era of Alzheimer’s disease. In the Alzheimer’s Association’s Facts and Figures, every 66 seconds someone is diagnosed with the disease and by year 2050, as many as 16 million could be affected. This has led to exciting research into basic pathology of the disease, forms of early detection such as the use of PET scans and new clinical medication trials.
While mental fitness is fluid and evolves over time, there are different forms of dementia and it is not necessarily an irreversible path to decline. There are new promises of chemicals and games for cognitive enhancement. For example, Lumosity, developed by neuroscientists, are fun games used to measure and enhance cognitive abilities in seniors. However, the lucrative billion dollar business of cognitive enhancers or “smart drugs” is controversial.
At Northwestern University, a group of my colleagues is studying superagers, older folks who have defied the normal cognitive decline. The hope is if we are able to figure out what’s different about their brains, maybe we can replicate it. For now, examining the imperfect and inadequacy of our understanding of mental fitness and the many ways we can approach its measurement can give us pause before we simply declare anyone has definitively achieved it.